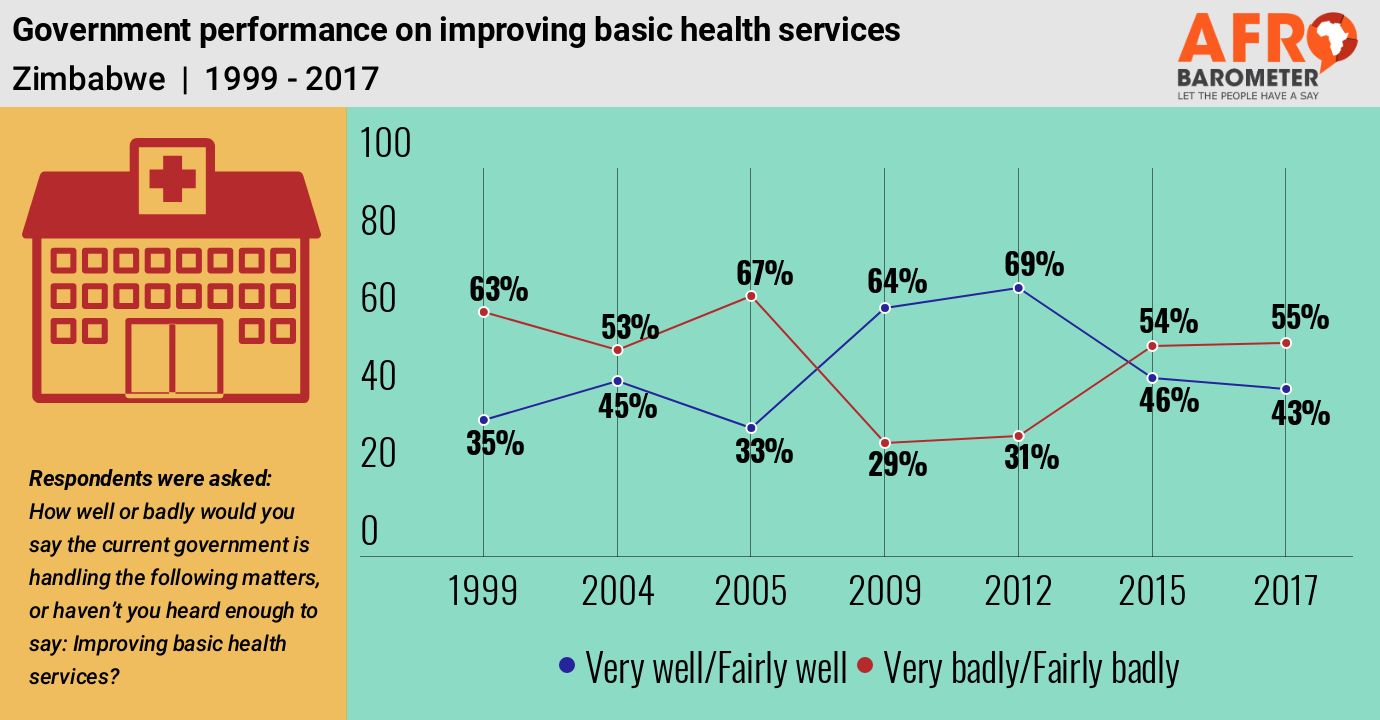
- A majority (55%) of Zimbabweans say the government is doing “fairly badly” or “very badly” at improving basic health services, more than 20 percentage points worse than evaluations in 2009 and 2012.
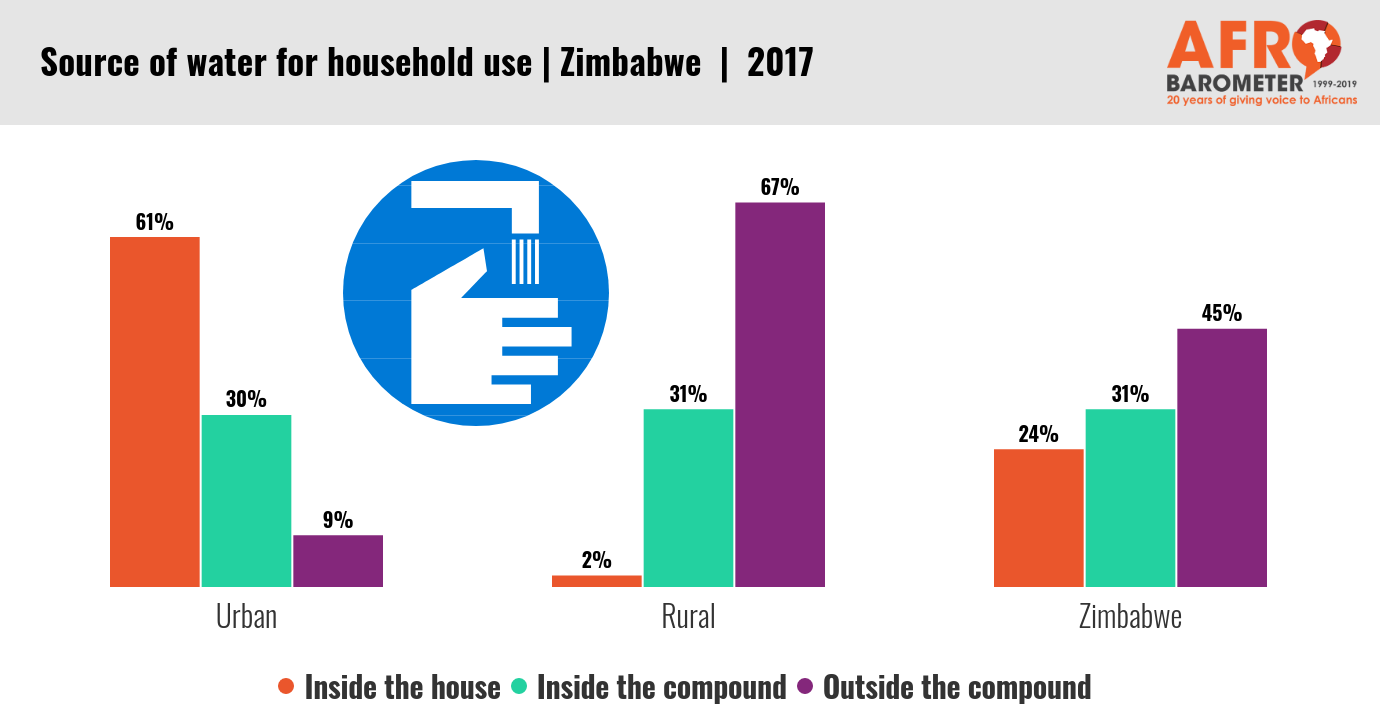
- Six in 10 Zimbabweans – but only five in 10 rural residents – live in areas with a nearby health clinic.
- A majority (59%) of respondents say they went without needed medicine or medical care at least once during the year preceding the survey. The proportion going without care decreased significantly between 2009 and 2012 but has remained stable since then.
- The same proportion (59%) say it is “difficult” or “very difficult” to obtain needed medical care. Poor respondents and urban residents are particularly likely to encounter difficulties.
- Only one-fourth (25%) of Zimbabweans say their ability to get needed health care has improved in recent years. Poor respondents and urbanites are more likely to say things have gotten worse than wealthier citizens and rural dwellers.
As Zimbabwe struggled to contain a deadly cholera outbreak in September-October 2018, questions focused again on failures of infrastructure and leadership that continue to leave the country vulnerable to such a preventable, “medieval” disease (Burke, 2018; Eyewitness News, 2018). Zimbabwe has suffered repeated cholera outbreaks, including one in 2008 that claimed more than 4,000 lives and infected more than 98,000 people (World Health Organization, 2009).
Fueled by poor sewage and water systems, the latest outbreak is also facilitated by inadequate health-care infrastructure and shortages of medicine, intravenous fluid, and protective clothing (World Health Organization, 2009, 2018; News24, 2018; Sunday Times, 2018). The government has declared a state of emergency, announced budget reallocations, and asked for international and private-sector assistance while politicians blame their opponents and several Harare City Council employees are accused of inflating prices on sanitary and health products (Burke, 2018; News24, 2018).
In this dispatch, we use Afrobarometer survey data collected in early 2017 to examine Zimbabweans’ perceptions of their health-care system. Findings show that citizens have become significantly more critical of the government’s performance on basic health care. Many Zimbabweans, especially poor and urban residents, say it’s difficult to obtain care, and a majority went without needed care at least once during the previous year.